Translate this page into:
Accuracy of transportal femoral aimer in placement of femoral tunnel during arthroscopic anterior cruciate ligament reconstruction: An observational study
*Corresponding author: Sushil Thapa, Department of Orthopaedics, Bharatpur Hospital, Bharatpur, Nepal. talktosus@gmail.com
-
Received: ,
Accepted: ,
How to cite this article: Thapa S, Joshi A, Singh N, Pradhan I, Kayastha N. Accuracy of transportal femoral aimer in placement of femoral tunnel during arthroscopic anterior cruciate ligament reconstruction: An observational study. J Arthrosc Surg Sports Med 2022;3:7-11.
Abstract
Objectives:
Incorrect placement of the femoral tunnel can result in failure of anterior cruciate ligament reconstruction. Several techniques have been described in literature to make accurate femoral tunnel. Although eyeballing and femoral offset aimer are commonly used, they are considered to be less accurate if used in isolation. To the best of our knowledge, no study has evaluated the use of combination of eyeballing and offset aimer to make the femoral tunnel. This study aims to evaluate the position of femoral tunnel made by combination of eyeballing and femoral offset aiming device.
Materials and Methods:
Post-operative radiographs of 50 patients were assessed. True anteroposterior (AP) and lateral view radiographs were used to evaluate the placement of the femoral tunnel using standard methods. The outcome was assessed and compared with the standard location of femoral tunnel as described by Harner et al. and Aglietti et al. Ease of making femoral tunnel and posterior blowout were recorded. Data analysis was performed using Statistical Package for the Social Sciences version 25 statistical analysis software.
Results:
In the coronal plane (AP view), the mean position of the femoral tunnel from the lateral cortex was at 35.09% ± 3.9% point. In AP plane (lateral view), the mean position of the femoral tunnel was at 80.01% ± 8.02% posteriorly along the Blumensaat’s line. None of the cases had posterior blowout and the technique was said to be easy.
Conclusion:
Eyeballing supplemented with transportal femoral offset aimer is an easy and accurate method of placing femoral tunnel and avoids posterior wall blowout.
Keywords
Accuracy
Anterior cruciate ligament reconstruction
Anatomic femoral tunnel
Transportal femoral aimer
INTRODUCTION
Malpositioned femoral tunnel is one of the most common causes of anterior cruciate ligament (ACL) reconstruction failure.[1-4] Various methods are described for making accurate inside out femoral tunnel. Eyeballing, arthroscopic ruler, Bernard-Hertel grid, and femoral offset guide are some of the popular ones.[5-8]
Use of Bernard-Hertel grid and arthroscopic ruler requires sophisticated instruments which may not be available easily. Eyeballing and femoral offset guide do not require sophisticated instruments but are considered less accurate.[9] Eyeballing to the footprint is simplest of all methods if it is done at 90° of knee flexion. However, visualization of same footprint is difficult in 130° of knee flexion as the anatomy is changed and the joint is more constrained, making eyeballing a difficult method. Femoral offset guide ensures adequate anteroposterior (AP) placement but poor in controlling superoinferior location, especially when the knee is hyperflexed, obscuring the anatomy of medial border of lateral femoral condyle. Hence, we planned to combine the eyeballing and femoral offset guide to create the anatomical femoral tunnel. The center of tunnel is marked at 90° flexion and the same point is targeted using the femoral offset guide.
There are no studies evaluating combination of eyeballing and offset guide in making femoral tunnel. We believe that the combination of these two methods is accurate, simple, and prevents posterior wall blowout. This study was conducted to evaluate the accuracy of femoral tunnel placement made by combining eyeballing and femoral offset methods.
MATERIALS AND METHODS
This is a prospective observational study, conducted over a period of 6 months (August 1, 2018–January 31, 2019). All patients undergoing transportal ACL reconstruction (ACLR) with hamstring graft were included in this study (convenient sampling). Patients undergoing revision ACLR, multiligament reconstruction, and reconstruction with transtibial technique were excluded from the study. Out of 62 patients eligible for study, we excluded 12 patients (7 had an improper lateral view and 5 lost to follow up [Figure 1].
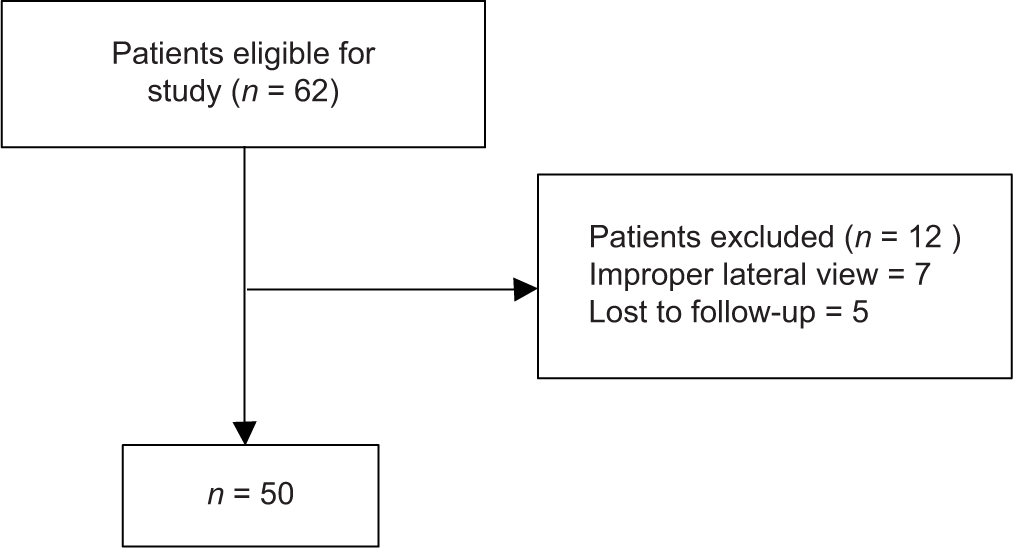
- Flowchart of patient selection.
Method of making femoral tunnel
After harvesting the hamstring graft and determining the size of the graft, a thorough diagnostic arthroscopy was performed through anterolateral (AL) and anteromedial (AM) portals. A far anteromedial (FAM) portal was created using a spinal needle in a manner that the reamer, when introduced through it, would not damage the cartilage while targeting the site of femoral tunnel.
Keeping the knee flexed at 90°, the site of femoral tunnel was marked with a radiofrequency ablator or microfracture awl by eyeballing. The mark was made at a point midway between the superior and inferior border of the lateral femoral condyle over the center of ACL femoral remnant. If remnant was completely absent, the bony landmark of resident’s ridge (lateral intercondylar ridge) is used and marking was done posterior to it. Shifting the arthroscope to AM portal, the location of marked area is verified. When arthroscope is in AL portal, knee is flexed to 130° to visualize the marked area. If it is not clearly visible, further debridement of remnant from femoral side is performed. Once the marked area was clearly visible at 130° of knee flexion, the offset aimer was introduced through FAM portal with the knee at 90° of flexion. A femoral offset of 6 mm was used for 8 mm graft and a 7 mm aimer was used for 9 mm graft. The hook of the aimer was placed posterior to the wall of lateral femoral condyle. Visualizing the marked point with arthroscope in AL portal, knee is flexed to 130°. A beath pin is inserted through the offset aimer and targeted toward the marking. The offset aimer is rotated up and down such that the guide wire’s tip (passing through the aimer) coincided with the mark made earlier by radiofrequency ablator or awl. If it did not coincide, the mark was reconsidered and marking was repeated to make sure it is in correct point. The guide wire tip should point at the marked area if the marking is correct and appropriate size of the offset aimer is used. Beath pin was then introduced through the marked point keeping the knee in 130° of flexion. Femoral tunnel drilling was performed over the beath pin.
Quadruple hamstring ACLR was performed with the standard technique in all cases. Femoral fixation was done with Endobutton or biodegradable interference screw. The tibial fixation of the graft was done using biodegradable interference screw.
At the 2nd post-operative week follow-up, true lateral and anteroposterior radiographic views of operated knee were obtained for radiological assessment of tunnel.
Radiological assessment
We took the measurements on the true AP and true lateral views. If the true AP or lateral view was not correctly taken, the radiograph was repeated since oblique views lead to the improper calculation of the positions of the midpoint of the tunnels. Calculation was performed using the Harner’s technique.[9,10]
Lateral radiograph
A true lateral view of the operated knee was obtained. Based on it, the position of the femoral and tibial tunnels was assessed using the methods described by Harner et al. [Figure 2].[9] A line was drawn from the anterior cortex to the posterior cortex along the Blumensaat line. The whole line was considered 100%. A point was identified and marked at the center of the tunnel’s beginning. The distance from the posterior cortex to the point was expressed in percentage across the Blumensaat line.

- Method of Harner et al. and Aglietti et al. for verification of femoral tunnel.
AP radiograph
On a true AP radiograph of the operated knee, the lateral and medial wall of the tunnel was identified. A center point of the tunnel was marked. The distances from the lateral femoral condyle to the center point of the tunnel were measured. Considering the intercondylar line as 100%, the distance from lateral condyle to center of tunnel was expressed in terms of percentage [Figure 3]. We compared our results against the reference in coronal plane as 42% (SD 3) from the lateral cortex and in AP plane as 83% (SD 4.7).[11,12]

- Illustration of the method of measuring the tunnel position on anteroposterior view.
Data analysis
A pro forma for each patient was filled with demographic data and details of radiographic measurement. The data were entered in the Statistical Package for the Social Sciences version 25 software. Using this software, the mean, standard deviation, and range of different variables were calculated.
RESULTS
There were all together 62 patients enrolled in the study. In seven patients, we could not locate the femoral tunnel clearly on lateral view even after repeating for 3 times. Another five patients lost to follow-up. Hence, these 12 cases were excluded from this study. Among 50 patients available for final analysis, 41 were male and only nine were female. The mean age of patients was 30.2 ± 7.7 years (ranging from 17 to 54 years).
On the lateral radiograph, 54% of the tunnel’s position was within 78.3–87.7% posteriorly along the Blumensaat’s line and 16% of the tunnels were more than 87.7% posteriorly [Table 1]. While in the AP radiograph, most (86%) of the tunnel’s position was <39% from the lateral femoral cortex and only 14% of them were within 39–45%.
| Tunnel position (Lat) | Number | Percentage of tunnels |
|---|---|---|
| <60% | 0 | 0% |
| 60–86% | 42 | 84% |
| >86% | 8 | 16% |
The mean tunnel position was 80.01% ± 8.02% posteriorly along the Blumensaat’s line on lateral radiograph views. Similarly, the mean tunnel position on the AP view was 35.09% ± 3.9% from the lateral cortex of the femoral condyle.
In all of these 50 cases, surgeon rated the process easy and there was no posterior blowout.
DISCUSSION
Non-anatomical placement of either tibial or femoral tunnel or both together has been associated with poor outcomes after ACLR.[13,14] Among these, malposition of the femoral tunnel is the most commonly reported cause of failure.[15] To improve the femoral tunnel placement, an outside in drilling technique has been described. However, this technique requires additional aiming device and a special drill bit which is expensive and requires additional surgical skills to use it.[15] Transportal, inside-out femoral drilling is most commonly performed method for making femoral tunnel. Since the drilling of femoral tunnel is done at 130° of knee flexion, it has to be done in very constrained space, and use of accessory instrument such as an arthroscopic ruler to locate the tunnel point is difficult. This is technically difficult even for an experienced arthroscopy surgeon.[16] Use of Hertel grid requires a C-arm with a special software of grid. This also increases the surgical time as well as brings large unsterile C-arm into the surgical field which increases the risk of infection.[7]
Eyeballing is by far the easiest technique, but it is difficult to get to the point at 130° which was marked at 90° of flexion. Since a longer beath pin is used to make the femoral tunnel, there is possibility of slippage of the beath pin and possibility of more posterior placement of the tunnel leading to posterior wall blowout.[5] A femoral offset aimer is very good technique to prevent the blowout and said to be accurate.[17] In another study done by Ellapparadja et al.,[17] they found that the contemporary over-the-top femoral tunnel guides did not provide sufficient offset to allow for an anatomical ACLR. This was because of high intersubject variability of femoral footprint in their subjects.[18] They also emphasized that the identification of remnant and making tunnel through the remnant is the most accurate method of making femoral tunnel.[18]
In this study, we combined two techniques (eyeballing and offset aimer) used to make the anatomical femoral tunnel. We marked the center of remnant, which is most anatomical location for femoral tunnel and used an offset aimer to aim tip of the beath pin to this point as a guide. The offset aimer secured adequate posterior wall and also prevented any advertent slippage of the beath pin.
In this study, the mean tunnel location in AP plane (lateral X-ray view) was at 80.01% [Table 3], which was similar to the study of Pinczewski et al. and Debnath et al.[11,19] In contrast to our study, Nema et al. placed femoral tunnels at an average of 69.41% ± 10.77% posterior along the Blumensaat’s line, which was more anterior to ours.[20] While in Pinczewski et al. study, the midpoint of the femoral tunnel was located at a mean of 86% ± 5% posteriorly along Blumensaat’s line, which was more posterior than our study.[11] Harner et al. in their study concluded that an ideal positioning of the femoral tunnel should be at approximately 80% of the AP length of the Blumensaat line, which was similar to our study.[9] Studies have recommended placing the femoral tunnel at least 60–86% posterior along the Blumensaat’s line.[11,19-21] Considering this fact, we can conclude that 84% of tunnel made by combination of eyeballing and femoral offset aimer are correctly placed.
In mediolateral plane (AP view of X-ray), the location of femoral tunnel was at 35.09% ± 3.9% medial to the lateral border of the femoral condyle [Table 3] which was lesser than other studies. Pinczewski et al.[11] found location of the tibial tunnel in the coronal plane at a mean of 46% ± 3% medial to the lateral border of the lateral femoral condyle.[11] The location of femoral tunnel in Nema et al. study was at a mean of 44.1% ± 3.9% medial to the lateral border of the lateral femoral condyle.[20] In a study by Debnath et al., in the coronal plane, the femoral tunnel location was at 43.2% ± 1.8% from the lateral condyle.[13] This difference may be because of the different technique of making femoral tunnel in our study. We did not use offset aimer blindly, rather we aimed for the marked footprint of the ACL in femur and used offset guide as a guiding device to reach to the marked spot.
Since, a positive correlation has been demonstrated between functional outcomes and posterior femoral tunnel placement on lateral radiographs [Table 2], we can conclude that all of our femoral tunnel were placed posteriorly in lateral radiograph.
| Tunnel position (AP) | Number | Percentage of tunnels |
|---|---|---|
| <39% | 43 | 86% |
| 39–45% | 7 | 14% |
| >45% | 0 | 0% |
AP: Anteroposterior
| Tunnel position coronal plane (AP view) | Tunnel position AP plane (lateral view) | |||||
|---|---|---|---|---|---|---|
| Mean | Range | Standard deviation | Mean | Range | Standard deviation | |
| Femur | 35.09 | 29–43 | 3.9 | 80.01 | 60–93 | 8.02 |
AP: Anteroposterior
Violation of the posterior femoral cortex, posterior wall blowout, can be a devastating intraoperative complication in ACLR and lead to loss of graft fixation or early graft failure.[22] Thus, an offset guide was recommended to use through an accessory anteromedial portal to place the tunnel anterior to the posterior margin of the femoral condyle.[23] There was no posterior wall blowout in our series as we secured the desired posterior wall using adequate size offset guide. The technique was also evaluated as easy to perform.
This study has some limitations. First, we did not always get a true lateral view of knee. Hence, we had to repeat to get appropriate lateral view. Second, on the AP view with the knee in extended position, the intercondylar notch overlaps with the exact entry point of the tunnel. Hence, the exact entry point was difficult to localize. This entry point could be better visualized in CT scan. We used radiolucent screws in all the patients. Hence, there’s likelihood of interobservers variability in assessing the tunnel position in the X-ray. A larger study, probably using a CT scan to calculate the tunnel position, is recommended.
CONCLUSION
Eyeballing supplemented with transportal femoral offset aimer is an accurate method of placing anatomical femoral tunnel. It is easy to perform and there is no complication of posterior wall blowout.
Declaration of patient consent
Institutional Review Board (IRB) permission obtained for the study.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
- Arthroscopic findings associated with roof impingement of an anterior cruciate ligament graft. Am J Sports Med. 1995;23:616-25.
- [CrossRef] [PubMed] [Google Scholar]
- Radiographic analysis of femoral interference screw placement during ACL reconstruction: Endoscopic versus open technique. Arthroscopy. 1993;9:154-8.
- [CrossRef] [Google Scholar]
- The relationship between the intercondylar roof and the tibial plateau with the knee in extension: Relevance for tibial tunnel placement in anterior cruciate ligament reconstruction. Arthroscopy. 1999;15:625-31.
- [CrossRef] [PubMed] [Google Scholar]
- Patient demographics and surgical characteristics in ACL revision: A comparison of French, Norwegian, and North American cohorts. Knee Surg Sports Traumatol Arthrosc. 2015;23:2339-48.
- [CrossRef] [PubMed] [Google Scholar]
- The effect of intraoperative fluoroscopy on the accuracy of femoral tunnel placement in single-bundle anatomic ACL reconstruction. Knee Surg Sports Traumatol Arthrosc. 2017;25:1211-8.
- [CrossRef] [PubMed] [Google Scholar]
- Validation of a new technique to determine midbundle femoral tunnel position in anterior cruciate ligament reconstruction using 3-dimensional computed tomography analysis. Arthroscopy. 2011;27:1259-67.
- [CrossRef] [PubMed] [Google Scholar]
- Femoral insertion of the ACL, Radiographic quadrant method. Am J Knee Surg. 1997;10:14-21.
- [Google Scholar]
- Femoral offset guide facilitates accurate and precise femoral tunnel placement for single-bundle anterior cruciate ligament reconstruction. Knee Surg Sports Traumatol Arthrosc. 2019;27:3505-12.
- [CrossRef] [PubMed] [Google Scholar]
- Anterior cruciate ligament reconstruction: Endoscopic versus two-incision technique. Arthroscopy. 1994;10:502-12.
- [CrossRef] [Google Scholar]
- Arthroscopically assisted semitendinosus and gracilis tendon graft in reconstruction for acute anterior cruciate ligament injuries in athletes. Am J Sports Med. 1996;24:726-31.
- [CrossRef] [PubMed] [Google Scholar]
- Radiological landmarks for placement of the tunnels in single-bundle reconstruction of the anterior cruciate ligament. J Bone Joint Surg Br. 2008;90:172-9.
- [CrossRef] [PubMed] [Google Scholar]
- Radiological analysis of bone tunnel position in anterior cruciate ligament reconstruction surgery: Comparison between the open technique and arthroscopy via an anteromedial portal. Rev Bras Ortop. 2011;46:270-5.
- [CrossRef] [PubMed] [Google Scholar]
- The relationship between tunnel placement and clinical results after anterior cruciate ligament reconstruction. Am J Sports Med. 1996;24:335-41.
- [CrossRef] [PubMed] [Google Scholar]
- Improperly placed anterior cruciate ligament grafts: Correlation between radiological parameters and clinical results. Knee Surg Sports Traumatol Arthrosc. 2000;8:207-13.
- [CrossRef] [PubMed] [Google Scholar]
- Causes for failure of ACL reconstruction and influence of meniscectomies after revision. Knee Surg Sports Traumatol Arthrosc. 2011;19:196-201.
- [CrossRef] [PubMed] [Google Scholar]
- Comparison of clinical results of anteromedial and transtibial femoral tunnel drilling in ACL reconstruction. BMC Musculoskelet Disord. 2020;21:1-7.
- [CrossRef] [PubMed] [Google Scholar]
- How to achieve an accurate anatomical femoral tunnel technique in ACL reconstruction in the early years of your consultancy? Femoral offset aimer technique: Consistent and reproducible technique. J Knee Surg. 2020;33:1201-5.
- [CrossRef] [PubMed] [Google Scholar]
- High variability in anterior cruciate ligament femoral footprint: Implications for anatomical anterior cruciate ligament reconstruction. Knee. 2021;30:141-7.
- [CrossRef] [PubMed] [Google Scholar]
- Radiological evaluation of tunnel position in single bundle anterior cruciate ligament reconstruction in the Indian population and their clinical correlation. J Clin Orthop Trauma. 2019;10:586-92.
- [CrossRef] [PubMed] [Google Scholar]
- Radiologic assessment of femoral and tibial tunnel placement based on anatomic landmarks in arthroscopic single bundle anterior cruciate ligament reconstruction. Indian J Orthop. 2017;51:286-91.
- [CrossRef] [PubMed] [Google Scholar]
- Radiographic findings in revision anterior cruciate ligament reconstructions from the Mars cohort. J Knee Surg. 2013;26:239-47.
- [CrossRef] [PubMed] [Google Scholar]
- Posterior wall blowout in anterior cruciate ligament reconstruction: A review of anatomic and surgical considerations. Orthop J Sport Med. 2016;4:2325967116652122.
- [CrossRef] [PubMed] [Google Scholar]






