Translate this page into:
Comparative effectiveness of myofascial release versus conventional physiotherapy in bicipital tendinopathy: A randomized controlled trial
*Corresponding author: Yakupiti Himan Shashidara De Silva, Sports Medicine Unit, National Hospital, Galle, Sri Lanka. drhiman1975@gmail.com
-
Received: ,
Accepted: ,
How to cite this article: De Silva YS, Thebuwanaarachchi ST, Gunawardena S, Samarawickrama M, De Silva OK, Perera HD. Comparative effectiveness of myofascial release versus conventional physiotherapy in bicipital tendinopathy: A randomized controlled trial. J Arthrosc Surg Sports Med. doi: 10.25259/JASSM_60_2024
Abstract
Objectives
Bicipital tendinopathy (BT) is considered one of the major differential diagnoses of anterior shoulder pain, often accompanied by a restricted or painful range of motion (ROM). Our objective was to assess the effectiveness of myofascial release (MFR) in alleviating pain and improving ROM in patients with BT.
Materials and Methods
Sixty participants were randomly assigned into two equal groups: A control group and an experimental/test group. The control group (30) received a pre-determined physiotherapy (PT) session. The test group (30) underwent three manual MFR therapy sessions every fifth day starting from day one. Pain during maximum ROM, by visual analog score, and degree of maximum ROM by a digital inclinometer were assessed 2 min before and 2 min after each intervention. Repeated-measures analysis of variance subsequently, the Bonferroni post hoc test was used to measure the statistical significance.
Results
Pain during ROM was measured on first day pre- and post-intervention, fifth day pre- and post-intervention, and on the tenth day pre- and post-intervention and as follows: 7.8 ± 0.4, 6.7 ± 0.4, 6.6 ± 0.4, 5.9 ± 0.4, 5.7 ± 0.4, and 5.4 ± 0.4, respectively. In the experimental group, the corresponding values were 7.6 ± 0.4, 5.3 ± 0.4, 4.6 ± 0.4, 3.7 ± 0.4, 3.4 ± 0.4, and 2.7 ± 0.4. compared to the baseline, both groups showed a significant improvement in pain scores after each session (P < 0.001). The baseline pain levels during ROM were similar between the control and experimental groups (P > 0.999). Those receiving MFR showed a significantly greater reduction in pain soon after each session, starting on day one (P < 0.001), compared to the conventional PT group. In addition, patients in the control group experienced a significant improvement in ROM, increasing from 169.9° ± 0.2.14° to 176.1° ± 1.15° (P < 0.01), whereas MFR improved ROM markedly from 150.1° ± 9.58° up to 180.0° ± 0.0° (P < 0.05).
Conclusion
MFR is more pronounced than conventional PT in alleviating painful shoulder ROM associated with BT.
Keywords
Bicipital
Digital dynamometer cum inclinometer
Myofascial release
Painful range of motion
Tendinopathy
INTRODUCTION
Background/rationale
Bicipital tendinopathy (BT) is commonly associated with overhead sports such as tennis, baseball, swimming, and weightlifting, where repetitive use of the shoulder places stress on the biceps tendon. It is also common among manual laborers involved in repetitive or strenuous shoulder activities. The prevalence of BT is difficult to isolate because it frequently accompanies other shoulder conditions, such as rotator cuff tears, impingement syndromes, and labral pathologies. The prevalence of shoulder pain in the general population is estimated to be between 7% and 26%, with a portion of these cases attributed to BT. Studies suggest that among athletes involved in repetitive overhead activities and older adults, the prevalence of BT can range between 10% and 30%.[1] As a degenerative condition, BT is more prevalent among individuals over the age of 40 due to the natural wear and tear of tendons, especially those with underlying shoulder conditions. BT includes a wide range of pathological conditions, from mild chronic-inflammatory tendinitis to more severe degenerative tendinosis, predominantly tendinopathy affecting the long head of the biceps tendon (LHBT). The reasons for the long head of the biceps (LHB) increased susceptibility compared to the short head of the biceps tendon remain unclear. LHBT conditions often coexist with many other shoulder pathologies. According to Nho et al., in 2010, the pathological changes leading to biceps LHB-tendinopathy involve an inflammatory cascade that begins with a chronic overuse injury, resulting in repetitive microtrauma within the LHBT.[2] This microtrauma results in the beginning of an initial acute inflammation within the LHBT. Over the time, continued microtrauma leads to degenerative changes, including the formation of adhesions and scar tissue, which restrict the mobility of the LHBT within the bony ligamentous bicipital canal. Consequently, the tendon itself becomes trapped within the grove. As depicted in Figure 1, this mechanical entrapment of the LHBT accounts for many of the symptoms and signs of the LHB-tendinopathy, including restricted range of motion (ROM), weakened shoulder forward flexion, as well as rest pain and or pain during movements. A comprehensive patient history, physical examination, and radiological investigations are essential for accurately diagnosing each of these conditions.[2]
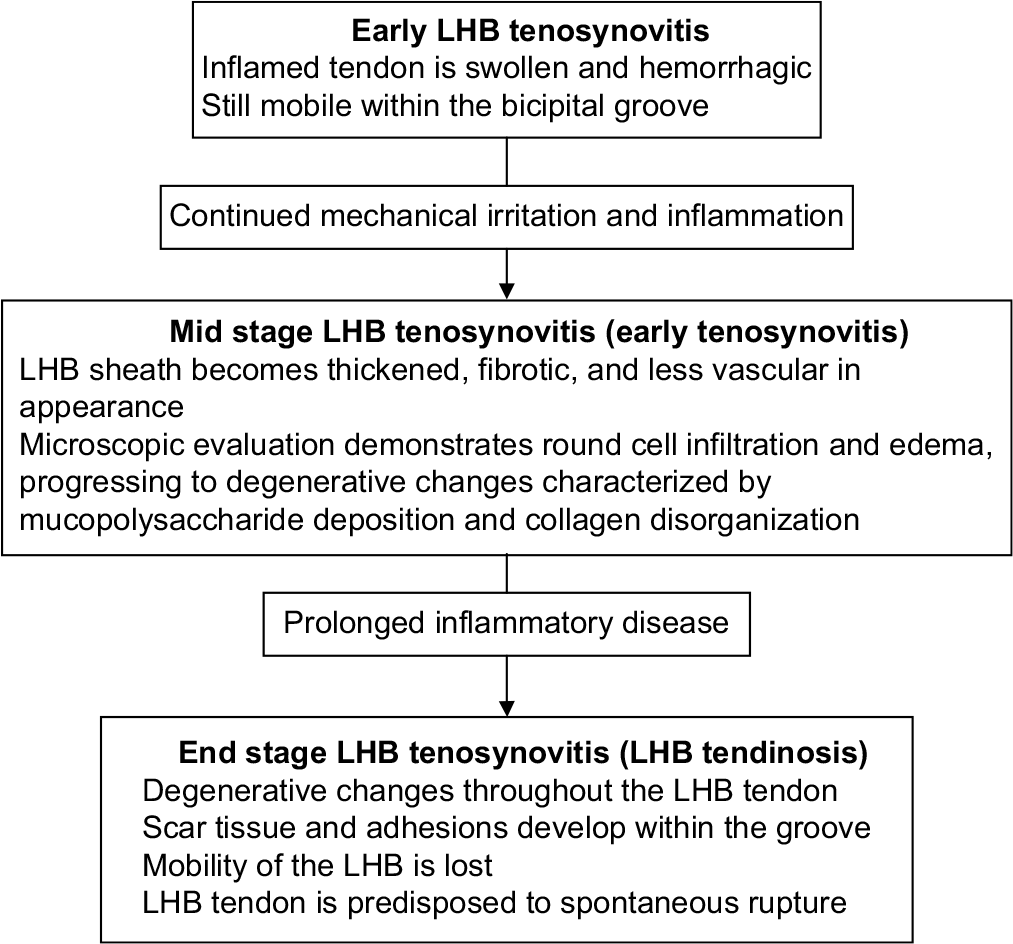
- The pathological changes leading to biceps brachii long head tendinopathy involves an inflammatory cascade. LHB: Long head of the biceps.
Murthi et al. highlighted the significance of incorporating the LHBT in a comprehensive treatment approach for shoulder impingement syndrome.[3] This recommendation highlights the need for a holistic approach to managing shoulder conditions, as addressing the LHB can significantly impact treatment outcomes for patients experiencing impingement symptoms.[3] Despite the variety of treatment options available, the prognosis for BT remains unsatisfactory. Treatment decisions for LHB issues are heavily influenced by coexisting shoulder conditions, as isolated LHB pathology is rare. The complexity of treatment choices is further compounded by a lack of robust clinical studies to provide clear guidance. There is a consensus on the need for well-designed research to more clearly outline the function of the LHBT in shoulder mechanics and to inform the best treatment approaches for various shoulder conditions.[4]
While there are growing anecdotal proofs supporting the effectiveness of myofascial release (MFR), research findings vary, and further studies are needed to establish standardized protocols and outcomes. The scientific literature reviews on the efficacy of MFR show variability in terms of both quality and outcomes. Despite these variations, the results from recent studies are encouraging, with emerging evidence supporting MFR as a promising approach. Although the quality of randomized controlled trials differs, recent publications have contributed to building a stronger evidence base for MFR. These studies offer a valuable foundation for future research, which will further clarify its effectiveness and optimize treatment protocols.[5] Therefore, this trial has been designed to fill two important gaps: first, formulation of an evidence-based optimum rehabilitation protocol for LHBT, and second, as per the previous research foundations and inferences to supplement the evidence for the effectiveness of MFR in treating LHBT.
Objective of the study
The objective was to assess the effectiveness of MFR in alleviating pain and improving ROM in patients with BT.
MATERIALS AND METHODS
Study design
It is a randomized control trial.
Setting
Sixty patients with long head of biceps tendinopathy from a sports and exercise medicine clinic of a tertiary care hospital were randomly assigned to control (30 patients) and experimental groups (30 patients). The control group underwent customary physiotherapy (PT), which included ultrasound therapy for 10 min and pre-designed ROM and strengthening exercises for 20 min on the 1st, 5th, and 10th days for three sessions over a 10-day period. The experimental group subjects were treated with three 30 min MFR sessions in a similar schedule, involving manual mobilization, pressure application, stretching, and rolling of soft tissues.
In addition, unless contraindicated, all subjects were given a conventional regimen of oral non-steroidal anti-inflammatory drugs.
Acetaminophen/paracetamol-1 g twice a day
Cox B inhibitor-celecoxib 200 mg twice a day
Proton pump inhibitor, omeprazole 20 mg twice a day.
Initial baseline measurements will be taken for all participants by an independent, trained staff member 2 min before the commencement of treatment on each day (either the clinic nurse or a physical therapist), focusing on eliminating the experimenter bias on the 1st day and in the future. Following this, the chief investigator would deliver the pre-planned experimental and control therapies to the participants according to a pre-determined schedule. Post-rehabilitation data and measurements will then be recorded by the same independent staff member within 2 min of the completion of the treatment at each relevant interval.
As shown in Figure 2, the pain levels during ROM of shoulder forward flexion (ROM-SFF) have been evaluated using the standard test instrument (visual analog scale [VAS]), the VAS for pain on 1st, 5th, and 10th days pre- and post-treatment, respectively.

- The standard test instrument for pain, Visual Analog Scale.
The VAS was used to assess participants’ pain intensity across multiple time points, providing a continuous and quantitative measure of changes over time. The 10 cm scale, ranging from “no pain” (0) to “worst possible pain” (10), allowed participants to mark their perceived pain levels. Its validity is reinforced by strong correlations with other standardized pain assessment tools, such as the Numeric Rating Scale and the McGill Pain Questionnaire. Widely validated in clinical and research settings, the VAS demonstrates high reliability and sensitivity to treatment effects, making it particularly suitable for musculoskeletal pain studies, including BT. Its ease of use reduces participant burden while maintaining robust pain assessment. To enhance study rigor, VAS measurements were taken at multiple time points, aligning with the repeated measures analysis of variance (ANOVA) design, improving statistical power, and providing a comprehensive analysis of pain progression and treatment efficacy. Standardized procedures and clear instructions further ensured the reliability and validity of the collected data.
The other test instrument depicted in Figure 3, the digital inclinometer by Hoggan Health, has been used to measure the ROM-SFF degree values on each respective date. On each of these days, both measurements (pain and ROMSFF) will be collected 2 min before and within 2 min after the intervention. The digital inclinometer was used to measure shoulder forward flexion ROM with high precision and reliability. Its objective digital readings minimize observer bias, making it preferable to traditional goniometers. Measurements were taken at multiple time points with standardized procedures to ensure consistency, accuracy, and repeatability. Each measurement was performed three times, with the average recorded for analysis. The device has demonstrated high intra- and inter-rater reliability, enhancing measurement consistency and also being sensitive enough to detect small but meaningful changes in ROM.
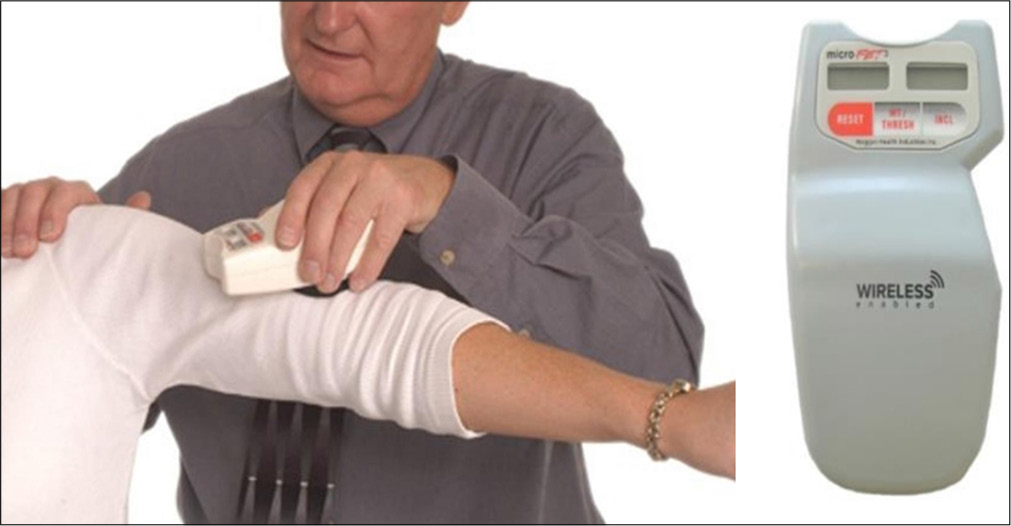
- Hand-held digital inclinometer-by Hoggan Health used to measure the range of motion of shoulder forward flexion (range of motion of shoulder forward flexion)
Participants and randomization
To achieve a balanced gender distribution between the control and experimental groups, stratified randomization was performed using computer-generated allocation through Statistical Package for the Social Sciences (SPSS) statistical software.
Inclusion criteria
Patients experiencing pain located in the anterior aspect of the shoulder with classical signs of LHBT tenderness in the bicipital canal when the shoulder is positioned in 10° of internal rotation from the anatomical position will be included in the study. The eligible age range will fall between 18 and 65 years, ensuring the exclusion of age-related muscle loss (sarcopenia).
Exclusion criteria
Patients presenting with the following shoulder conditions or other health concerns will be excluded:
Fractures, malignancies, neurological conditions, for example, cervical radiculopathy, soft-tissue disorders, for example, polymyalgia rheumatica and bleeding diathesis, and acute dermatological conditions, for example, rash, infections
In addition, the exclusion applies to those who have undergone MFR on the shoulder within the last 14 days, are non-consenting, or have any contraindications for MFR (whether total or local).
Diagnoses of LHBT among patients from a sports and exercise medicine clinic of a tertiary care hospital were confirmed by clinical evaluation of both a standalone specialist rheumatologist and a specialist orthopedic surgeon. Patient recruitment will follow those criteria.
If both shoulders are affected, the study will focus on the more severely impacted shoulder based on patient assessment, while both shoulders will follow an identical treatment method.
Variables
There were two outcome variables measured; VAS pain score during maximum shoulder forward flexion and the maximum degree of ROM-SFF; values expected were fallen between 0–10 and 0°–180°, respectively. The raw values of quantitative variables were analyzed.
Data sources/management
Both control and experimental group variables were measured by the same trained staff, and the test instruments and the comparability of the assessment method were maintained.
Bias
There could be two potential sources of bias, and each has been dealt with to minimize. The diagnostic error has been minimized by an independent double diagnosis of LHBT by both a specialist rheumatologist and an orthopedic surgeon. The interventions were done by the principal investigator. Focusing on eliminating the experimenter bias, the baseline measurements and follow-up measurements were taken for all participants by an independent, trained staff member and either the clinic nurse or a physical therapist 2 min before the commencement of treatment on each day. Thus, bias has been addressed at three different points by intervening with their standalone investigators.
Study size
The sampling approach used is purposive sampling.
The G Power 3.1 was used for the calculation of accurate sample size, which is widely recommended for calculating accurate sample size for studies, particularly when the prevalences are unknown. The software is free of charge and can be downloaded from the internet. Moreover, the decision to use G*Power was based on its capability to perform power analysis, which helps determine the minimum number of participants required to obtain reliable and valid results while minimizing the risk of Type I (false positive) and Type II (false negative) errors. The sample size estimation took into account several key factors, including the effect size (set at 0.305 to represent the expected magnitude of the difference between groups), the significance level (a), typically set at 0.05, the power (1-b), which is commonly set at 80% or 0.80 to detect a true effect, and the allocation ratio between the control and experimental groups, which was set at 1:1. In addition, the analysis considered three measurements and used a repeated measures ANOVA for the statistical test. Using G*Power 3.1, a sample size of 60 was determined to ensure sufficient power for detecting meaningful differences while maintaining statistical rigor and avoiding issues with underpowered or excessively large samples.
Statistical method
Version 25 of the IBM SPSS software has been used for data compiling and analysis. The statistical significances were determined by repeated-measures ANOVA and subsequently by the Bonferroni post hoc statistical analytical test.
Ethical approval and patient consent
Approval has been granted by the Ethics Review Committee of the Faculty of Medicine, University of Ruhuna, Galle, Sri Lanka (No. 2020.P.126). In addition, the Sri Lanka Clinical Trials Registry has registered the research under the serial number SLCTR/2022/002 and approved the intervention procedures.
All patients have consented in writing to participate in the study.
RESULTS
Participants
There were 87 patients with shoulder pain examined for eligibility. Sixty patients were confirmed as having LHBT, and all were included in the study. No dropouts were encountered during the period of 10 days of follow-up.
Descriptive data
The control group comprised 21 males and nine females, with a mean age of 35.3 ± 15.4 years. Meanwhile, the intervention group comprised 20 males and 10 females, with an average age of 35.5 ± 13.4 years. There was not any statistically significant difference in mean ages, which was found between the groups.
The average duration of the shoulder pain for the control group was 35.7 ± 18.1 days and 36.8 ± 18.7 days for the experimental group, indicating no significant difference in duration.
Main results
Pain during ROM in the control group on 1st day pre- and post-intervention, 5th day pre- and post-intervention, and on 10th day pre- and post-intervention were as follows: 7.8 ± 0.4, 6.7 ± 0.4, 6.6 ± 0.4, 5.9 ± 0.4, 5.7 ± 0.4, and 5.4 ± 0.4, respectively. In the experimental group, the corresponding values were 7.6 ± 0.4, 5.3 ± 0.4, 4.6 ± 0.4, 3.7 ± 0.4, 3.4 ± 0.4, and 2.7 ± 0.4. compared to the baseline, both groups showed a significant improvement in pain scores after each session (P < 0.001) [Table 1].
| VAS Pain score while ROM-SFF | 1st Day before intervention | 1st Day after intervention | 5st Day before intervention | 5st Day after intervention | 10th Day before intervention | 10th Day after intervention | Statistical significance |
|---|---|---|---|---|---|---|---|
| Pain during ROM-SFF (Control) | 7.8±0.4 | 6.7±0.4 | 6.6±0.4 | 5.9±0.4 | 5.7±0.4 | 5.4±0.4 | P<0.001 RM ANOVA |
| Pain during ROM-SFF (Intervention) | 7.6±0.4 | 5.3±0.4 | 4.6±0.4 | 3.7±0.4 | 3.4±0.4 | 2.7±0.4 | P<0.001 RM ANOVA |
ROM-SFF: Range of motion in shoulder forward flexion, VAS: Visual analogue scale, RM ANOVA: Repeated measures analysis of variance.
The baseline pain levels during ROM were similar between the control and experimental groups (P > 0.999). Those receiving MFR showed a significantly greater reduction in pain soon after each session, starting on day 1 (P < 0.001), compared to the conventional PT group. In addition, patients in the control group experienced a significant improvement in ROM, increasing from 169.9° ± 0.2.14° to 176.1° ± 1.15° (P < 0.01), whereas MFR improved ROM markedly from 150.1° ± 9.58° up to 180.0° ± 0.0° (P < 0.05) [Table 2].
| **Degrees of ROM while SFF | 1st Day before intervention | 1st Day after intervention | 5st Day before intervention | 5st Day after intervention | 10th Day before intervention | 10th Day after intervention | Statistical significance |
|---|---|---|---|---|---|---|---|
| ROM- SFF0 (Control-PT) | 169.90±2.140 | 172.80±1.650 | 173.50±1.530 | 174.40±1.320 | 174.30±1.280 | 175.10±1.150 | P<0.01 RM ANOVA |
| ROM- SFF0 (Intervention-MFR) | 150.10±9.580 | 168.40±4.450 | 170.80±3.870 | 178.30±0.870 | 178.90±0.590 | 180.00±0.00 | P<0.05 RM ANOVA |
DICUSSION
Key results
Rehabilitating LHB tendinopathy poses a significant challenge for the sports medicine team since the condition often resists conventional treatments.[6] This condition is debilitating, significantly impairing the performance of athletes, especially those involved in overhead repetitive throwing and frequent heavy lifting sports.[7,8] Apart from pathological explanation, most of the clinical signs and symptoms could primarily be due to physical restriction of the altered LHB tendon. Tendon en routes first inside the pulley system and thereafter within the bicipital canal. The end results will hinder or entrap the fine, smooth gliding movements of the fibro-cartilaginous section of the LHBT.[9-11] The condition is typically managed through experience-based rather than evidence-based practices, and it is frequently misdiagnosed as adhesive capsulitis. This study aims primarily to evaluate the effectiveness of MFR as a primary PT approach for rehabilitating LHB tendinopathy, based on the evidence subsequently to develop an empirical rehabilitation guideline.
Moreover, the study proposes that myofascial theory and understanding of the anatomy of the fascial planes may offer a biomechanical rationale for successful myofascial therapies in addressing LHB tendinopathy. The myofascial theories can help not only in understanding pain patterns but also in identifying specific, strategic areas for targeted treatment. The study specifically determines the potential effectiveness of myofascial manipulation in addressing chronic anterior shoulder pain caused by LHB tendinopathy, a widespread issue. A key aspect of this approach is its focus on assessing and treating exact anatomical and biomechanical sites where patients report feeling pain and the pathology exists.
In a 2009 anatomical study by Day et al., it was demonstrated that the continuous connection of fascia across the posterior upper limb is maintained by muscles attaching to this connective tissue, creating an integrated myofascial pathway from one end of the limb to the other.[12] Therefore, it is reasonable to propose that the pain patterns and limitations in ROM associated with LHB tendinopathy could result from significant adhesions formed between the myofascial structures surrounding the LHBT pathway. When the extracellular matrix of the deep fascia shifts from a solid to a gel-like state, such as from overuse syndromes, strain, or repetitive stress injuries, it affects the ability of the endofascial collagen fibers to glide smoothly against each other. This alteration leads to increased stiffness. This may result in two outcomes: first, a mechanical or tensional response, and second, a potential disruption in afferent signaling causing reduced ROM and pain, respectively.[12]
Other researchers suggest that restoring the dimensions and integrity of myofascial tissue may alleviate pressure on nociceptive structures like neurovascular tissues while also enhancing the alignment and mobility of the joints.[12-14]
The fascial manipulation technique aims to restore the smooth movement of collagen and elastic fibers within the ground substance by utilizing the heat produced from deep manipulation friction.[14] The average time to reduce pain by half was 3.24 min. However, for subjects with symptoms lasting less than 3 months (sub-acute cases), the average time was shorter at 2.58 min, compared to 3.29 min for chronic patients.[15] Figure 4 depicts the MFR techniques used in the study. Manual techniques such as deep kneading of the muscular fascia at specific points, called centers of coordination and centers of fusion along myofascial pathways, have demonstrated positive results. Treating a proximal point over the deep fascia, along with a distal point, has been effective in reducing pain and enhancing mobility. This suggests that it may not always be necessary to treat the entire myofascial chain to alleviate widespread myofascial pain.[12] Figure 4 (a-e) shows a hands-on manual therapy technique to release myofascial tissues to reduce pain and improve tissue mobility.
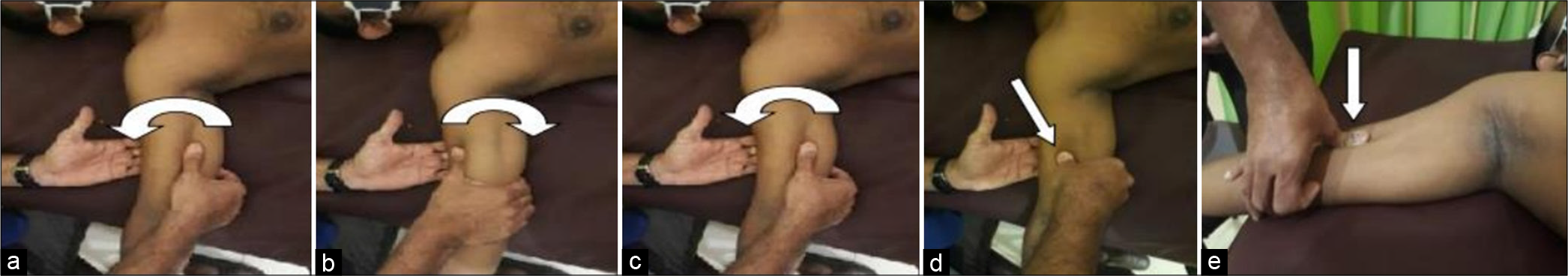
- (a-e) A hands on manual therapy technique to release mayofascial tissues to reduce pain and improve tissue mobility. Curved arrows in (a), (b), and (c) depicts the directions of thumb motion back and forth during MFR. Straight arrows in (d) and (e) shows the downward pressure applied during MFR.
The results from Tables 1 and 2 suggest that the intervention group, which received MFR treatment, exhibited more significant enhancements in pain relief and ROM in comparison to the control group, which received only standard PT. These findings highlight the potential benefits of incorporating MFR as a first-line adjunct therapy for managing LHB tendinopathy.
Pain management
As shown in Table 1, both groups experienced a decrease in pain over the 10-day period, but the intervention group demonstrated a more significant reduction. On day 1, both groups started with similar baseline pain scores (6.7 ± 0.29 for the control group and 6.60 ± 0.35 for the intervention group). However, by Day 10, the intervention group’s pain scores dropped to 2.56 ± 0.25, while the control group reached 4.43 ± 0.27. This greater reduction in pain for the intervention group suggests that MFR may accelerate pain relief compared to standard treatments alone. This finding aligns with previous studies showing that MFR can be effective in reducing pain in musculoskeletal conditions, particularly in chronic cases where traditional methods may not provide sufficient relief.
ROM improvement
In terms of ROM, Table 2 highlights the increased forward flexion in the intervention group compared to the control group. The intervention group showed significant gains from baseline to Day 10, demonstrating a much larger improvement than the control group. This suggests that MFR, when combined with conventional PT, enhances the flexibility and mobility of the shoulder joint, likely by addressing the myofascial restrictions that limit movement. Further, Graph 1 depicts the progression in shoulder forward flexion ROM during the 10-day treatment period for both the control and intervention groups. In the control group on day 1, the baseline ROM for forward flexion was recorded. By day 5, there was a slight increase in ROM, both before and after the intervention. Further, moderate improvement was noted by day 10, but the overall change from day 1 to day 10 remained relatively modest. When a similar outcome was observed in the intervention group, it displayed a significantly enhanced improvement in ROM relative to the control group. Initial measurements on day 1 showed restricted movement, but by day 5, there was a notable increase in ROM before and after the intervention sessions. By day 10, substantial gains were observed, indicating a greater overall increase in ROM from the baseline.
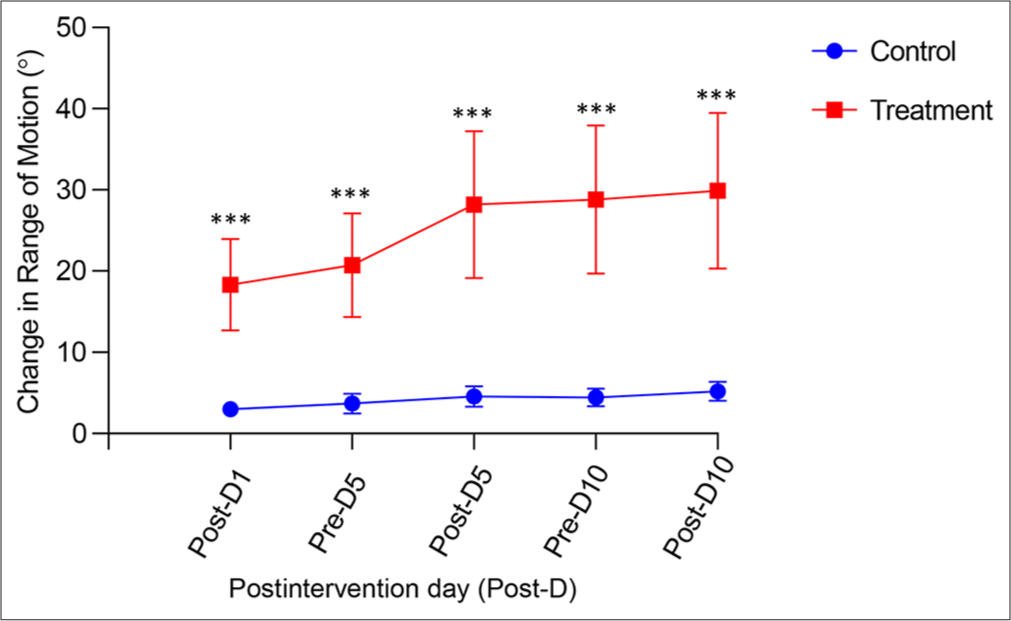
- The difference of degrees (0) of shoulder flexion from baseline from 1st day to 10th day. This graph shows the improvement of shoulder forward flexion from the benchmark for both in the control and interventional groups over time. ***highly significant difference.
While the statistical significance of the findings demonstrates clear differences between the groups, addressing the clinical significance is essential to understand the practical impact of these changes. The significant pain reduction observed in the MFR group (P < 0.001) suggests that MFR provides rapid and meaningful relief, which could translate to improved function and quality of life for patients. In addition, the substantial improvement in ROM in the MFR group (from 150.10 ± 9.580 to 180.00 ± 0.00) indicates a full restoration of shoulder mobility, which is particularly relevant for individuals with BT who struggle with daily activities requiring overhead movement. In contrast, while the conventional PT group also showed a statistically significant increase in ROM (from 169.90 ± 2.140 to 176.10 ± 1.150, P < 0.01), the improvement was less pronounced compared to the MFR group. From a clinical perspective, the near-complete restoration of ROM in the MFR group suggests that MFR may be more effective in achieving functional recovery, particularly for patients with restricted movement. These findings reinforce the potential of MFR as a valuable intervention, not only for reducing pain but also for enhancing functional outcomes in patients with shoulder impairments.
Clinical implications of the study
Relevance of findings
The findings that MFR is more effective than conventional PT in reducing pain and improving ROM for patients with BT can influence treatment protocols and clinical decision-making in PT practice.
Treatment approaches
The study suggests that incorporating MFR into treatment plans for patients with BT may lead to better outcomes. Clinicians might consider incorporating MFR as a complementary therapy alongside standard approaches.
Broader application
The study’s implications extend beyond BT, suggesting MFR as a potentially valuable modality for various shoulder-related conditions. This could prompt further investigations into its efficacy for other shoulder pathologies.
Future research
The paper opens avenues for future studies to explore long-term impacts of MFR, effects on different populations (athletes versus non-athletes), and the combination of MFR with other therapeutic modalities.
Limitations and strength
Despite the significant findings, this study has certain limitations that should be acknowledged. One key limitation is the short follow-up period, which may not fully capture the long-term effects of MFR and conventional PT on pain reduction and ROM improvement. While the immediate and short-term benefits are evident, it remains unclear whether these gains are sustained over weeks or months. Future studies with extended follow-up periods are needed to determine the long-term efficacy and durability of these interventions. To check on the recurrence and prognosis of the condition, it would be better to review the patients in 6-month intervals for at least two years. This amount of follow-up is difficult. Another potential limitation is the presence of confounding factors that could have influenced the results. Variability in patients’ daily activities, adherence to prescribed home exercises, and differences in baseline muscle tension or inflammation levels may have affected the outcomes. While efforts were made to standardize treatment protocols, individual differences in response to therapy could not be entirely controlled. In addition, the study focused on a specific population with BT, which may limit the generalizability of the findings to individuals with other shoulder conditions. The inclusion of only two treatment groups (MFR and PT) also restricts comparisons with other potential interventions, such as combined therapies or pharmacological approaches. Finally, observer bias could be a factor, as the assessors were aware of the treatment groups. Although objective measurement tools such as the digital inclinometer and VAS were used, blinding of evaluators could further enhance the study’s validity in future research. Addressing these limitations in future studies will help strengthen the evidence base for MFR and its role in musculoskeletal rehabilitation. The main strengths of the study are a high number of participants, the use of high accurate hand-held digital goniometer to take measurements, and uninterrupted follow-up. On the contrary, the lack of comparable studies made it difficult to benchmark the results. In the future, more research on this clinical condition has to be conducted to find more evidence, especially the efficacy of rehabilitation of LHBT with a combination of MFR with several other PT modalities.
CONCLUSION
MFR proves to be more effective than conventional PT for BT, leading to a greater reduction in VAS pain scores and ROM. Further research is needed to investigate the precise mechanisms behind these improvements.
Acknowledgment
This research work was undertaken as a partial fulfillment of the requirements for a PhD degree at the University of Ruhuna, Sri Lanka, by Dr. Y.S.H. De Silva. We would like to express our gratitude to Dr. D. Jayasekara. M.D. (VOS), Dr. S.P. Dissanayake. M.D. (CR) assisting the conformation of the cases. Dr. Shelton Perera. M.D. (Director) National hospital, granting approval for the data collection. Dr. Minhan M.A.M, Prof. Karunanayake A, Prof. Weeraratne T.P for their contributions in data collection, process, and analysis.
Author contributions
YHSD: Conceptualized and designed the study, ensuring its scientific rigor and relevance; OKLS and HMDP: Actively involved in data collection, statistical analysis, and initial result interpretation; STT, MBS and SG: Contributed to the comprehensive interpretation of findings and took the final result interpretation and texting.
Ethical Approval
The research/study approved by the Institutional Review Board at Ethics Committee of the Medical faculty of the government university of Sri Lanka-Ruhuna, number 2020.P.126 (November 20, 2020), dated February 17, 2021.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent.
Conflicts of interest
There are no conflicts of interest.
Use of artificial intelligence (AI)-assisted technology for manuscript preparation
The authors confirm that there was no use of artificial intelligence (AI)-assisted technology for assisting in the writing or editing of the manuscript and no images were manipulated using AI.
Financial support and sponsorships: Nil.
References
- Incidence and prevalence of poststroke shoulder pain among different regions of the world: A systematic review and meta-analysis. Fron Neurol. 2021;12:724281.
- [CrossRef] [PubMed] [Google Scholar]
- Long head of the biceps tendinopathy: Diagnosis and management. J Am Acad Orthop Surg. 2010;18:645-56.
- [CrossRef] [PubMed] [Google Scholar]
- The incidence of pathologic changes of the long head of the biceps tendon. J Shoulder Elbow Surg. 2000;9:382-5.
- [CrossRef] [PubMed] [Google Scholar]
- Long head of biceps: From anatomy to treatment. Acta Reumatol Portuguesa. 2015;40:26-33.
- [Google Scholar]
- Effectiveness of myofascial release: Systematic review of randomized controlled trials. J Bodyw Mov Ther. 2015;19:102-12.
- [CrossRef] [PubMed] [Google Scholar]
- Tendinopathy of the long head of the biceps. Med Sport Sci. 2012;57:76-89.
- [CrossRef] [PubMed] [Google Scholar]
- Long head of the biceps tendon pain: Differential diagnosis and treatment. J Orthop Sports Phys Ther. 2009b;39:55-70.
- [CrossRef] [PubMed] [Google Scholar]
- Diagnosis and treatment of biceps tendinitis and tendinosis. Am Fam Physician. 2009;80:470-6.
- [Google Scholar]
- 'The origin of the long head of the biceps from the scapula and glenoid labrum An anatomical study of 100 shoulders. J Bone Joint Surg Br. 1994;76-B:951-4.
- [CrossRef] [Google Scholar]
- Mechanical properties of the long head of the biceps tendon. Knee Surg Sports Traumatol Arthrosc. 1996;3:226-9.
- [CrossRef] [PubMed] [Google Scholar]
- Functional anatomy of the shoulder. Phys Ther. 1966;46:1043-51.
- [CrossRef] [PubMed] [Google Scholar]
- Application of fascial manipulation technique in chronic shoulder pain-anatomical basis and clinical implications. J Bodyw Mov Ther. 2009;13:128-35.
- [CrossRef] [PubMed] [Google Scholar]
- Myofascial release of carpal tunnel syndrome. J Am Osteopath Assoc. 1993;93:92-4-100-1.
- [CrossRef] [Google Scholar]
- Fasciatherapy combined with pulsology touch induces changes in blood turbulence potentially beneficial for vascular endothelium. J Bodyw Mov Ther. 2009;13:239-45.
- [CrossRef] [PubMed] [Google Scholar]
- How much time is required to modify a fascial fibrosis? J Bodyw Mov Ther. 2010;14:318-25.
- [CrossRef] [PubMed] [Google Scholar]







