Translate this page into:
Peroneus longus autograft with lateral extra-articular tenodesis for revision anterior cruciate ligament surgery has excellent short-term outcomes
*Corresponding author: Manit Arora, Department of Orthopaedics and Sports Medicine, Fortis Hospital, Mohali, Punjab, India. jvshah03@gmail.com
-
Received: ,
Accepted: ,
How to cite this article: Arora M, Shah J. Peroneus longus autograft with lateral extra-articular tenodesis for revision anterior cruciate ligament surgery has excellent short-term outcomes. J Arthrosc Surg Sports Med. doi: 10.25259/JASSM_6_2025
Abstract
Objectives
Revision of failed anterior cruciate ligament (ACL) surgery has consistently shown poorer clinical outcomes and lower return to sport rates than the primary ACL surgery. We investigated the clinical outcomes of using a peroneus longus (PL) graft for revision ACL surgery combined with a lateral extra-articular tenodesis procedure.
Materials and Methods
Institutional ethics approval was obtained before the initiation of the study. Thirty consecutive patients were prospectively recruited with clinical and radiological evidence of ACL reconstruction failure and followed up for a one-year duration. Knee outcomes (Visual Analog Scale [VAS], International Knee Documentation Committee (IKDC) and Lysholm) scores, return to sport rates, ankle outcome measures (American Orthopedic Foot and Ankle score and functional ankle disability index), and complications were assessed.
Results
All thirty patients were males with an average age of 28.9 ± 4.4 years. One third of the study population comprised athletes. Excellent knee and ankle outcomes were observed, with significant improvement in VAS, IKDC, and Lysholm scores over the study duration. The re-rupture rate in the entire study population was 7%, with a return to sport rate of 93% and a return to sport at a pre-injury level of 73% at an average duration of 10.8 months post-surgery.
Conclusion
The use of PL graft combined with lateral extra-articular tenodesis in revision ACL surgery provides excellent clinical outcomes with a high return to sport rate and a low complication rate.
Keywords
Anterior cruciate ligament
Lateral extra-articular tenodesis
Outcomes
Peroneus longus
Revision anterior cruciate ligament
INTRODUCTION
Rupture of the anterior cruciate ligament (ACL) and its subsequent surgical reconstruction has been associated with high failure rates (as high as 20% in some studies) with a multi-factorial etiology and lack of consensus regarding optimum graft choice and fixation methods in the revision setting.[1] The decision to opt for a revision ACL surgery is both technically demanding for the surgeon and a burden for the patient. Graft options for revision ACL surgery are similar to primary ACL surgery: Bone-based grafts (such as bone patellar tendon bone [BPTB] and allograft) and soft tissue-based grafts (hamstring, quad tendon, and peroneus longus [PL]).
Revision of a failed ACL surgery has consistently shown poorer clinical outcomes and lower return to sport rates than primary ACL surgery,[2-6] with only 40-50% of patients returning to sport at a pre-injury level after revision surgery,[7] significantly lower rates when compared to primary surgery. Although a variety of factors[1,2] have been elucidated as potential causes of this reduced functional outcomes and lower return to sport (RTS), including lower quadriceps strength, concomitant damage to the knee, and ensuing osteoarthritis in the revision groups, one of the common findings of the Norwegian and Danish registry data has been the poorer outcomes with hamstring autografts in revision ACL surgery.[1]
In lieu of this, we explored using PL autograft, which has been shown to have better graft diameters than hamstring grafts,[8,9] as our graft choice for revision ACL surgery in the present prospective cohort study. There is no study in the literature, to the authors’ knowledge, that has examined using PL for revision ACL surgery. In addition, we added a lateral extra-articular tenodesis (LET) to provide better rotational control to the revised knee.[10,11] Our hypothesis is that the combination of a larger reliable graft diameter with the peroneal graft and the pivot control offered by the LET will lead to a more stable knee in the revision setting.
MATERIALS AND METHODS
Patient recruitment
We performed a prospective cohort study at a tertiary referral center of 30 consecutive patients entering the service for the treatment of primary ACL surgery failure between January 2022 and January 2023. Institutional ethics approval was obtained from the institutional ethics review committee prior to the initiation of the study (July 2021). The study conforms to the guidelines set forth in the Declaration of Helsinki.
The inclusion criteria [Table 1] were patients over the age of 18 years with a demonstrated complete ACL graft tear on clinical testing and magnetic resonance imaging (MRI) willing to participate in the study and give written informed consent. Patients with tunnel diameters on computed tomography imaging <12 mm were included. Patients with concomitant injuries to the medial meniscus or lateral meniscus, cartilage defects, and lack of varus or valgus malalignment were included. Patients with Kellgren-Lawrence osteoarthritis of grade II or below were included.
| Inclusion criteria | Exclusion criteria | |
|---|---|---|
| Age | Patients over the age of 18 years | Patients under the age of 18 years |
| Clinical and MRI finding | Complete ACL graft tear (concomitant injuries to meniscus and cartilage were included) | Multi-ligament injuries (including combined MCL and ACL injuries) |
| Tunnel diameter on CT imaging | <12 mm | 12 mm or above |
| Willing to participate and give informed consent | Yes | No |
| Varus or valgus alignment on standing scanograms | No | Yes |
| Increased posterior tibial slope on long leg lateral Xray | No | Yes |
| Kellgren-Lawrence Osteoarthritis Grade | I and II | III and IV |
Kellgren-Lawrence Osteoarthritis Grade I and II III and IV MRI: Magnetic resonance imaging, CT: Computed tomography, ACL: Anterior cruciate ligament, MCL: Medial collateral ligament
Exclusion criteria were those with multi-ligament injuries (including combined medial collateral ligament [MCL] and ACL injuries), those with tunnel diameters more than 12 mm, those unwilling to participate or give written informed consent, and those with age <18 years. Patients with varus or valgus malalignment or increased posterior tibial slope, which required a corrective osteotomy procedure, were excluded, as were patients with Kellgren-Lawrence osteoarthritis grade III or IV.
Study power calculation
Using a correlation coefficient of 0.04 to study the null hypothesis, we found that the sample size should be 48 patients for a moderately high power and reduced error rate. Using 30 patients, the alpha score is <0.05, showing moderate power and fair error rate.
Surgical procedure
A single surgeon (MA) performed the procedure. Standard single-stage revision ACL reconstruction was performed using a PL graft, our preferred graft choice for primary ACL surgeries.[12] We use an adjustable loop endobutton (Stryker©, USA) on the femur, a tripled PL graft (average graft diameter: 9 mm ± 0.6 mm), and a PEEK screw (Arthrex©, USA) on the tibial side. No tapes were used for augmentation or internal bracing. Concomitant injuries such as meniscal injuries and chondral injuries were addressed using the appropriate techniques at the same time.
For the lateral extra-articular procedure (LEAP), we use a modified deep Lemaire LET technique with a 6cm leaflet of the iliotibial band of 1cm width, freed proximally and whipstitched. The lateral collateral ligament was identified and the leaflet is tunneled under it and up to the insertion point (just proximal and posterior to the lateral epicondyle). We used an anchor (Omega™, Stryker©, USA) for fixing the LET and angle the direction of insertion parallel to the femur tunnel of the ACL to avoid tunnel coalition. Violation of the ACL femoral tunnel was checked before tightening by viewing from the anteromedial portal. We fixed the LET graft at 30° of knee flexion and neutral rotation with 20-30 Newtons of applied force and checked for further tightening in the deeper degrees of knee flexion. The position of 30° of flexion is used as per current evidence[13] to prevent residual laxity or overtensioning of the graft. Once fixed, the ACL graft was passed and secured under direct arthroscopic vision.
The post-operative rehabilitation protocol comprised passive straight leg raise, passive knee flexion, and vastus medialis oblique development from day 1. Weight bearing was prohibited for the first 2 weeks, patients were made partial weight bearing in week 3 and full weight bearing in week 4. Range of motion (ROM) time frames were 0-30° in week 1, 30-60° in week 2, 60-90° in week 3, and 90-further in week 4. A knee immobilizer was used for the first 3 weeks after surgery, after which the patient was shifted to a functional ACL brace for a total of 3-month post-surgery. Thereafter, a phased recovery protocol was followed.
Rehabilitation plays a vital role in returning the athlete to sport. A phased rehabilitation protocol was adopted with each phase criteria being met prior to shifting the patient to the next phase of rehab.[14] In addition, at the end of the rehab cycle, return to sport testing consisting of muscle strength testing and hop tests were performed before clearing the patient for return to sport.[15]
Data collection
All patients were screened at baseline for demographic variables (age, gender, and player/non-player), MRI outcomes (meniscal, chondral, and ligamentous injuries), radiological outcomes (grade of osteoarthritis, posterior tibial slope, varus or valgus malalignment), pain scores (VAS - Visual Analog Scale), and functional knee scores (IKDC and Lysholm scores). In addition, as we use PL graft for harvest, we have also included ankle outcome scores (American Orthopaedic Foot and Ankle Score [AOFAS] and Functional Ankle Disability Index [FADI]). Baseline data was entered into a master sheet by one of the authors (JS) throughout the study period.
Patients were followed up routinely at 6 weeks, 3-month, 6-month, and 1-year post-surgical intervention for functional outcome measures (IKDC and Lysholm score), pain scores (VAS), ankle outcome scores (AOFAS and FADI), and clinical testing (ROM, Anterior drawer, Lachman and pivot shift tests). Complications such as persistent pain, subjective instability, infection, neurovascular complaints, stiffness, and others were also recorded. Return to sport times after completion of muscle testing using a dynamometer and hop tests were also recorded. Return to sport and return to sport at a pre-injury level along with patient satisfaction were also assessed using a subjective patient-centric questionnaire which asked questions like: “Are you satisfied with the procedure?”, “Would you recommend the procedure to a friend suffering from the same injury?”, “Have you returned to sport?”, and “Have you returned to sport at the same level at which you were playing before the injury?”
The follow-up testing was done by both the lead author (MA). All data were entered into the master sheet at each visit by JS. Data synthesis and statistical analysis of data were performed by the main author (MA).
Statistical analysis of data
The statistical analysis was performed using IBM Statistical Package for the Social Sciences 20 software. Descriptive statistics (mean and standard deviation) were calculated for VAS, IKDC, Lysholm, AOFAS, and FADI and were used in the data evaluation to summarize the sample. Depending on the observed distribution, the paired t-test was used to evaluate the associations between time intervals and scores. Repeated measures analysis of variance (RM ANOVA) analysis was used to test inter-subject significance between study groups for sub-variables and study outcomes. The age sub-variable was divided into those below the age of 30 years and those above the age of 30 years. As the study had no female patients, sub-group analysis for gender was not performed. The significance level adopted was P < 0.05.
RESULTS
All thirty patients completed the study duration with no dropouts. Descriptive data of the entire study population is presented in Table 2. The study was heavily biased towards male patients with no females recruited during the study duration. Half the study population was below 30 years of age, and half was above 30 years of age. The majority of the study population comprised players (64%), those who play sports at a non-recreational level. Recreational athletes constituted only one-third of the study population.
Pre-operative MRI and X-ray findings of the study cohort are presented in Table 3. The majority of patients had associated meniscal or chondral pathologies at the time of presentation. Medial meniscus tears (73%) were more common than lateral meniscus tears (23%). A total of eight patients had undergone a meniscal procedure (meniscectomy or meniscal repair) in their index surgery, out of which three had a failed meniscal repair and one had a successful meniscal repair. The remaining four patients had a meniscectomy procedure, which showed no signal changes on MRI. Diffuse chondral wear pattern in a compartment was seen in six patients with the medial compartment being affected in the majority. Localized chondral defects on MRI were observed in one-third of the study population with the medial compartment being affected in the majority of patients. Of note, 40% of the study cohort had radiographic evidence of Grade I or II osteoarthritis.
| Variable | Count | Minimum | Maximum | Mean | Standard deviation |
|---|---|---|---|---|---|
| Age group | |||||
| <30 years | 15 | ||||
| 30+years | 15 | ||||
| Sex | |||||
| Male | 30 | ||||
| Player | |||||
| No | 11 | ||||
| Yes | 19 | ||||
| Patient demand | |||||
| Low-demand | 10 | ||||
| High-demand | 20 | ||||
| Age | 30 | 20 | 39 | 28.9 | 4.36 |
| Pre-op-VAS R | 30 | 0 | 6 | 2.8 | 2.63 |
| Pre-op-VAS A | 30 | 0 | 8 | 3.9 | 2.95 |
| Pre-op-VAS S | 30 | 0 | 6 | 1.8 | 2.16 |
| Pre-op-IKDC | 30 | 54 | 78 | 69.2 | 5.91 |
| Pre-op-Lysholm | 30 | 76 | 90 | 81.5 | 4.74 |
| Pre-op-AOFAS | 30 | 100 | 100 | 100.0 | 0.00 |
| Pre-op-FADI | 30 | 104 | 104 | 104.0 | 0.00 |
| Post-op: 3-month VAS R | 30 | 0 | 1 | 0.1 | 0.25 |
| Post-op: 3-month VAS A | 30 | 1 | 3 | 1.8 | 0.55 |
| Post-op: 3-month VAS S | 30 | 0 | 1 | 0.1 | 0.25 |
| Post-op: 3-month IKDC | 30 | 72 | 83 | 78.9 | 2.33 |
| Post-op: 3-month Lysholm | 30 | 78 | 92 | 86.9 | 4.24 |
| Post-op: 3-month AOFAS | 30 | 96 | 100 | 99.6 | 1.22 |
| Post-op: 3-month FADI | 30 | 100 | 104 | 103.2 | 1.63 |
| Post-op 6-month scores-VAS R | 30 | 0 | 0 | 0.0 | 0.00 |
| Post-op 6-month scores-VAS A | 30 | 1 | 1 | 1.0 | 0.00 |
| Post-op 6-month scores-VAS S | 30 | 0 | 0 | 0.0 | 0.00 |
| Post-op 6-month scores-IKDC | 30 | 72 | 86 | 82.8 | 3.21 |
| Post-op 6-month scores-Lysholm | 30 | 78 | 100 | 91.7 | 5.65 |
| Post-op 6-month scores-AOFAS | 30 | 100 | 100 | 100.0 | 0.00 |
| Post-op 6-month scores-FADI | 30 | 104 | 104 | 104.0 | 0.00 |
| Post-op 1-year scores -VAS R | 30 | 0 | 1 | 0.1 | 0.25 |
| Post-op 1-year scores-VAS A | 30 | 0 | 2 | 0.7 | 0.60 |
| Post-op 1-year scores-VAS S | 30 | 0 | 0 | 0.0 | 0.00 |
| Post-op 1-year scores-IKDC | 30 | 62 | 86 | 81.7 | 5.74 |
| Post-op 1-year scores-Lysholm | 30 | 88 | 96 | 93.3 | 2.19 |
| Post-op 1-year scores-AOFAS | 30 | 100 | 100 | 100.0 | 0.00 |
| Post-op 1-year scores-FADI | 30 | 104 | 104 | 104.0 | 0.00 |
AOFAS: American Orthopaedic Foot and Ankle Score, FADI: Functional Ankle Disability Index, VAS R: Visual Analog Scale at Rest, VAS A: Visual Analog Scale at activity, VAS S: Visual Analog Scale at sleep, IKDC: International Knee Documentation Committee Score
| Imaging variable | Yes (n) | No. (n) | Positive imaging finding as percentage of study cohort |
|---|---|---|---|
| Complete ACL graft tear | 30 | 0 | 100% |
| Medial meniscus tear | 22 | 8 | 73% |
| Lateral meniscus tear | 7 | 23 | 23% |
| Failed meniscal repair (in index surgery) | 3 (2 medial, 1 lateral) | 27 (22 had no meniscal procedure performed in index surgery, 5 had a menisectomy or meniscal repair which showed no changes) | 10% |
| Chondral wear diffuse in any compartment on MRI | 6 (5 medial, 1 lateral, 2 patellofemoral) | 24 | 20% |
| Chondral defect/s isolated on MRI | 10 (9 medial, 1 lateral, 2 patellofemoral/trochlea) | 20 | 33% |
| Failed cartilage procedure in index surgery | 2 (2 previous microfractures) | 28 (27 had no cartilage procedure performed, 1 had a successful microfracture done previously) | 7% |
| Kellgren-Lawrence OA Grade I/II | 12 | 18 | 40% |
Kellgren-Lawrence OA Grade I/II 12 18 40% MRI: Magnetic resonance imaging, ACL: Anterior cruciate ligament, OA: Osteoarthritis
Assessment of the entire study population scoring data is presented in Graph 1, Tables 4 and 5. There is a significant improvement in all scoring parameters when compared to the baseline and at each follow-up duration through the study. Further, the strength of the significance (P < 0.001) is strong across the majority of endpoints in paired calculation. Ankle outcomes report no significant differences except at one time point, as most patients return to full ankle outcomes (as with baseline) by the 3-month mark.
| Mean | VAS R | VAS A | VAS S | IKDC | Lysholm | AOFAS | FADI |
|---|---|---|---|---|---|---|---|
| Pre-operative | 2.8 | 3.9 | 1.8 | 69.2 | 81.5 | 100.0 | 104.0 |
| 3 months | 0.1 | 1.8 | 0.1 | 78.9 | 86.9 | 99.6 | 103.2 |
| 6 months | 0.0 | 1.0 | 0.0 | 82.8 | 91.7 | 100.0 | 104.0 |
| 1 year | 0.1 | 0.7 | 0.0 | 81.7 | 93.3 | 100.0 | 104.0 |
| Standard Deviation | VAS R | VAS A | VAS S | IKDC | Lysholm | AOFAS | FADI |
| Pre-operative | 2.6 | 3.0 | 2.2 | 5.9 | 4.7 | 0.0 | 0.0 |
| 3 months | 0.3 | 0.6 | 0.3 | 2.3 | 4.2 | 1.2 | 1.6 |
| 6 months | 0.0 | 0.0 | 0.0 | 3.2 | 5.7 | 0.0 | 0.0 |
| 1 year | 0.3 | 0.6 | 0.0 | 5.7 | 2.2 | 0.0 | 0.0 |
AOFAS: American Orthopaedic Foot and Ankle Score, FADI: Functional Ankle Disability Index, VAS R: Visual Analog Scale at Rest, VAS A: Visual Analog Scale at activity, VAS S: Visual Analog Scale at sleep, IKDC: International Knee Documentation Committee Score
| Paired differences | t | df | Sig. (2-tailed) | ||||||
|---|---|---|---|---|---|---|---|---|---|
| Mean | Std. deviation | Std. error mean | 95% confidence interval of the difference | ||||||
| Lower | Upper | ||||||||
| Pair 1 | Pre-op-VAS R -Post-op: 3-month VAS R | 2.767 | 2.712 | 0.495 | 1.754 | 3.780 | 5.587 | 29 | 0.000 |
| Pair 2 | Pre-op-VAS R -Post-op 6-month scores-VAS R | 2.833 | 2.627 | 0.480 | 1.852 | 3.814 | 5.907 | 29 | 0.000 |
| Pair 3 | Pre-op-VAS R -Post-op 1-year scores -VAS R | 2.767 | 2.555 | 0.467 | 1.812 | 3.721 | 5.930 | 29 | 0.000 |
| Pair 4 | Pre-op-VAS A -Post-op: 3-month VAS A | 2.100 | 3.078 | 0.562 | 0.951 | 3.249 | 3.737 | 29 | 0.001 |
| Pair 5 | Pre-op-VAS A -Post-op 6-month scores-VAS A | 2.900 | 2.952 | 0.539 | 1.798 | 4.002 | 5.381 | 29 | 0.000 |
| Pair 6 | Pre-op-VAS A -Post-op 1-year scores -VAS A | 3.200 | 3.418 | 0.624 | 1.924 | 4.476 | 5.128 | 29 | 0.000 |
| Pair 7 | Pre-op-VAS S -Post-op: 3-month VAS S | 1.733 | 2.227 | 0.407 | 0.902 | 2.565 | 4.262 | 29 | 0.000 |
| Pair 8 | Pre-op-VAS S -Post-op 6-month scores-VAS S | 1.800 | 2.156 | 0.394 | 0.995 | 2.605 | 4.573 | 29 | 0.000 |
| Pair 9 | Pre-op-VAS S -Post-op 1-year scores -VAS S | 1.800 | 2.156 | 0.394 | 0.995 | 2.605 | 4.573 | 29 | 0.000 |
| Pair 10 | Pre-op-IKDC -Post-op: 3-month IKDC | −9.667 | 6.950 | 1.269 | −12.262 | −7.072 | −7.618 | 29 | 0.000 |
| Pair 11 | Pre-op-IKDC -Post-op 6-month scores-IKDC | −13.600 | 7.127 | 1.301 | −16.261 | −10.939 | −10.451 | 29 | 0.000 |
| Pair 12 | Pre-op-IKDC -Post-op 1-year scores -IKDC | −12.533 | 9.504 | 1.735 | −16.082 | −8.984 | −7.223 | 29 | 0.000 |
| Pair 13 | Pre-op-Lysholm -Post-op: 3-month Lysholm | −5.400 | 4.174 | 0.762 | −6.959 | −3.841 | −7.086 | 29 | 0.000 |
| Pair 14 | Pre-op-Lysholm -Post-op 6-month scores-Lysholm | −10.233 | 7.842 | 1.432 | −13.162 | −7.305 | −7.148 | 29 | 0.000 |
| Pair 15 | Pre-op-Lysholm -Post-op 1-year scores -Lysholm | −11.867 | 5.788 | 1.057 | −14.028 | −9.705 | −11.230 | 29 | 0.000 |
| Pair 16 | Pre-op-AOFAS -Post-op: 3-month AOFAS | 0.400 | 1.221 | 0.223 | −0.056 | 0.856 | 1.795 | 29 | 0.083 |
| Pair 19 | Pre-op-FADI -Post-op: 3-month FADI | 0.800 | 1.627 | 0.297 | 0.192 | 1.408 | 2.693 | 29 | 0.012 |
Significant changes are highlighted in green. AOFAS: American Orthopaedic Foot and Ankle Score, FADI: Functional Ankle Disability Index, VAS R: Visual Analog Scale at Rest, VAS A: Visual Analog Scale at activity, VAS S: Visual Analog Scale at sleep, IKDC: International Knee Documentation Committee Score, df: Degrees of freedom, t: t-statistic value
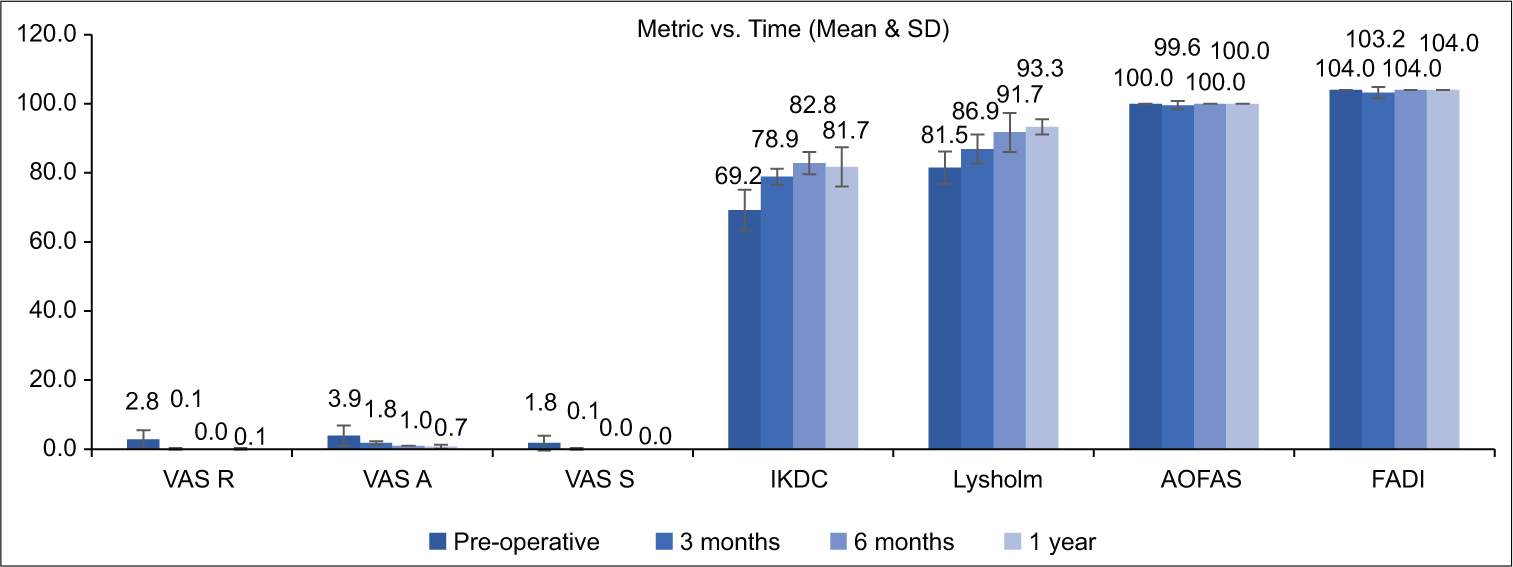
- Graphical representation of entire study population outcomes data over the study duration. AOFAS: American orthopaedic foot and ankle score, FADI: Functional ankle disability index, VAS R: Visual Analog Scale at Rest, VAS A: Visual Analog Scale at activity, VAS S: Visual Analog Scale at sleep, IKDC: International knee documentation committee score. SD: Standard deviation.
Subgroup analysis
RM ANOVA analysis was performed using sub-group variables (age, player/non-player, and low demand/high demand). Players had significantly higher AOFAS scores at 3 months (P = 0.015) versus non-players, but this equalized by the 6-month follow-up. Further, higher-demand patients had significantly lower Lysholm scores (P = 0.020) at 3 months compared to lower-demand patients, but this again equalized by the 6-month follow-up. Apart from these, there were no significant differences observed across the study duration for any scores when compared to sub-group variables.
RM ANOVA analysis was also performed to compare chondral and meniscal injuries versus no chondral and no meniscal injuries, respectively. There were no significant differences observed for study outcome measures across the study duration for these sub-group variables.
Return to sport
The average rate of return to sport was 10.8 months (range: 9.2-11.8; standard deviation: 0.4). Of the entire study population, 28 patients (93%) returned to sport (either recreational or non-recreational), and 22 patients (73%) returned to the sport at a pre-injury level [Graph 2]. Specifically focusing on the player cohort (n = 19 patients), we found that the return to sport occurred in 18 patients (95%), with a return to sport at pre-injury level in 12 patients (63%).
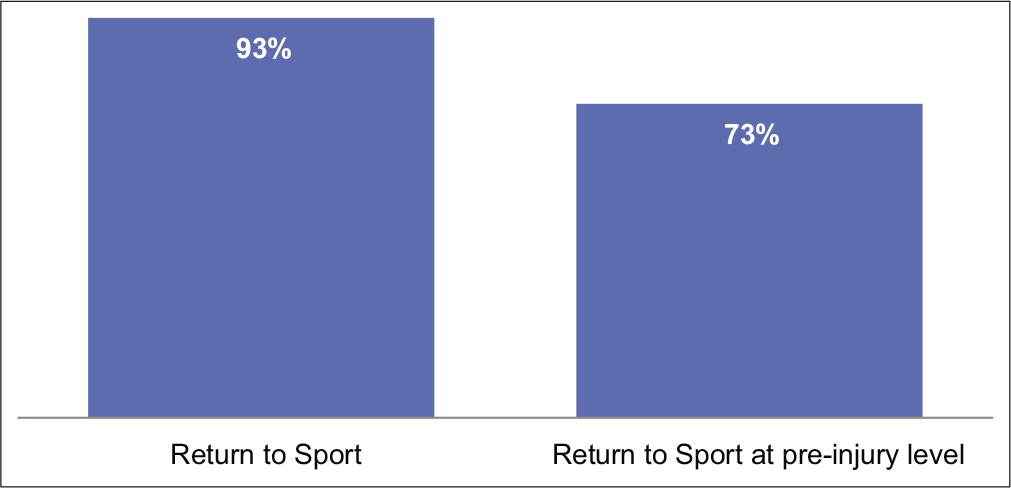
- Return to sport and return to sport at pre-injury level rates for the entire study population (n = 30 patients).
Complications
Of the entire study population, two patients (7%) had a feeling of subjective laxity at the end of 1-year follow-up, with one showing a partial ACL graft tear on repeat MRI and one showing a complete ACL graft tear. There were no MRI-based failures of the LET. No patient had an infection of the knee post-surgery. One patient had a superficial wound infection to the PL harvest site, which resolved with daily dressings and a short course of antibiotics. No patient complained of stiffness in the knee.
Specific to the LET, three patients (10%) complained of lateral-sided knee pain at the LET site at 3 months, which may represent the ensuing fibrosis process or possibly over-constraint. Two of these complaints were resolved by 6 months, with only one patient complaining of ongoing lateral-sided knee pain at 1-year follow-up, with low VAS scores. The most common complication related to the LET procedure was the shape change phenomenon[16] which was observed in eight patients (27%) at 1-year follow-up.
DISCUSSION
Rupture of the anterior cruciate ligament (ACL) and its subsequent surgical reconstruction has been associated with high failure rates (as high as 20% in some studies). The decision to opt for a revision ACL is both technically demanding and a burden for the patient. Unfortunately, as with primary ACL surgery, there exists a lack of consensus amongst surgeons with regard to graft choice, tunnel drilling, and fixation methods in revision cases.[1] A systematic review and meta-analysis of revision anterior cruciate ligament reconstruction (ACLR)[17] highlighted the heterogeneous graft choices in revision ACL surgery, dictated by the availability of either host or allograft tendons, which invariable leads to heterogeneous surgical outcomes and lack of consensus as to optimal graft choice. Although many surgeons advocate for bone-based grafts (BPTB or allograft with bone plug) in the setting of revision ACLR, the outcomes have shown negligible superiority to soft tissue grafts.[17] Accordingly, the present study set out to investigate the clinical outcomes of using PL graft, our choice for primary ACL surgery, in the revision setting in combination with a lateral extra-articular tenodesis procedure. Recent research work by our group has shown that PL graft harvest has both, minimal impact on ankle functional outcome scores[18] and on ankle biomechanics.[19]
A meta-analysis of graft choices in revision ACL surgery found that autografts perform superior to allografts, but within the autograft options, there is not much difference in clinical outcomes.[20] It is this lack of consensus and the poorer outcomes with hamstring autograft revisions in the Norwegian and the Danish[1] that has stimulated the search for more reliable autografts. Contrastingly, in our study, we found both better clinical outcome scores for the knee and better pain scores when compared to the meta-analysis data. Further work is needed to assess the outcomes of PL grafts in revision cases, especially in a larger cohort and for a longer study duration.
In their comparative study of patellar tendon versus quadriceps tendon versus hamstring tendon autografts for revision ACL surgery, Meena et al. found similar clinical outcomes with an average re-rupture rate of approximately 10% across the groups.[21] Not only did our study show superior clinical outcomes to the before-mentioned data, but the graft re-rupture rate in our study population was slightly lower (7%). Similar cohort sizes were used in each arm of Meena et al.’s study when compared to our present study suggesting cross-comparability of data.[21]
Revision of a failed ACL surgery has consistently shown poorer clinical outcomes and lower return to sport rates than primary ACL surgery,[2-6] with only 40-50% of patients returning to sport at a pre-injury level after revision surgery,[7] significantly lower rates when compared to primary surgery. A recent systematic review[22] showed a high return to sport rates after revision ACLR, but when looking at the RTS to pre-injury level, these rates were much lower (<60% of patients), and there was also a high re-rupture rate (approximately 20%). The current study found RTS rates much higher than the available literature (73% of patients returned to the sport at a pre-injury level), which may be due to the sparing effect that PL grafts have on the quadriceps and hamstrings (as neither is touched during the revision procedure) enabling better maintenance of muscle mass and hence accelerating the rehab pathway and providing a possible protective role of these agonists and antagonist of the ACL.
The concept of anterolateral rotatory instability (ALRI) has evolved and gained acceptance in recent years.[23-25] LEAPs are particularly indicated for correcting ALRI in revision cases, especially in high-demand and high-pivot athletes.[26] The combined procedure of ACLR with LEAP has high RTS rates (75-85%) comparable to primary ACLR.[27] This indicates that the addition of a lateral procedure may not compromise the ability of an athlete to return to a pre-injury level, and on the other hand probably does not speed up the return to sport either. In their comparative study, Rayes et al. found similar clinical outcomes for BPTB with LET versus hamstring tendon with anterolateral ligament reconstruction.[28] Our study found superior outcomes and higher RTS rates for PL with LET when compared to their similarly sized cohort. However, a difference was found in complication rates with a higher complication rate in our present study, especially related to the LET procedure. The factoring in of the newly described shape change phenomenon likely contributed to this higher complication rate, a complication which was not assessed in the before mentioned study.
The present study does have limitations. The first and most important limitation is the small sample size, which is underpowered to identify major differences in functional outcomes compared to the literature but comparable to individual armed cohorts of previous studies using other graft options. Revision ACL reconstruction is a less commonly performed procedure than primary ACL reconstruction, and as such the volume of cases is lower. Second, the follow-up duration has been limited to a year; however, longer-term data is needed to assess for long-term graft survival. Third, the lack of a comparative arm means that all inferences are inter-study rather than intra-study. Further, only males were included in the study as during the study period, only males presented fitting the inclusion criteria. This does introduce gender bias.
The clinical relevance of the present study is important. Against the backdrop of increasing revision ACL rates globally, there is a need for more viable autograft options. The present prospective cohort study has shown promise for PL in this setting as a viable graft option with better clinical outcomes compared to the literature and superior return to sport rates. A follow-up of the study with comparative arms to the patellar tendon, quadriceps tendon, and/or hamstring tendon grafts will yield more insight.
CONCLUSION
Autograft options in revision ACL surgery are as abundant as in primary ACL surgery, largely based on surgeon preferences. The literature has consistently shown poorer clinical outcomes with revision ACL surgery and lower return to sport rates, irrespective of graft selection. The present prospective cohort study, when compared to the available literature, shows superior clinical outcomes with the use of PL graft in revision settings with a higher return to sport rate. A direct comparative study of PL with other graft options will add more insight.
Author contributions
MA: Conceptualized the manuscript, statistical analysis, and was the primary author; JS: Involved in data collection and editing of the manuscript.
Ethical approval
The research/study was approved by the Institutional Review Board at Fortis Hospital Mohali, number IRB - 2022/11, dated 2022.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent.
Conflicts of interest
There are no conflicts of interest.
Use of artificial intelligence (AI)-assisted technology for manuscript preparation
The authors confirm that there was no use of artificial intelligence (AI)-assisted technology for assisting in the writing or editing of the manuscript and no images were manipulated using AI.
Financial support and sponsorship: Nil.
References
- Factors associated with revision following anterior cruciate ligament reconstruction: A systematic review of registry data. Knee. 2020;27:287-99.
- [CrossRef] [PubMed] [Google Scholar]
- Revision ACL reconstruction with autograft: Long-term functional outcomes and influencing factors. Eur J Orthop Surg Traumatol. 2019;29:157-61.
- [CrossRef] [PubMed] [Google Scholar]
- Inferior results after revision ACL reconstructions: A comparison with primary ACL reconstructions. Knee Surg Sports Traumatol Arthrosc. 2013;21:2011-8.
- [CrossRef] [PubMed] [Google Scholar]
- Does revision ACL reconstruction measure up to primary surgery? A meta-analysis comparing patient-reported and clinician-reported outcomes and radiographic results. Br J Sports Med. 2016;50:716-24.
- [CrossRef] [PubMed] [Google Scholar]
- What Is the mid-term failure rate of revision ACL reconstruction? A systematic review. Clin Orthop Relat Res. 2017;475:2484-99.
- [CrossRef] [PubMed] [Google Scholar]
- Outcome after anterior cruciate ligament revision. Curr Rev Musculoskelet Med. 2019;12:397-405.
- [CrossRef] [PubMed] [Google Scholar]
- Revision anterior cruciate ligament reconstruction: Clinical outcome and evidence for return to sport. Knee Surg Sports Traumatol Arthrosc. 2015;23:2825-45.
- [CrossRef] [PubMed] [Google Scholar]
- Peroneus longus tendon autograft versus hamstring tendon autograft in anterior cruciate ligament reconstruction: A comparative study with a mean follow-up of two years. Arch Bone Jt Surg. 2022;10:695-701.
- [Google Scholar]
- Peroneus longus tendon autografts have better graft diameter, less morbidity, and enhanced muscle recuperation than hamstring tendon in ACL reconstruction. Indian J Orthop. 2024;58:979-86.
- [CrossRef] [PubMed] [Google Scholar]
- Effect of lateral extra-articular tenodesis on the rate of revision anterior cruciate ligament reconstruction in elite athletes. Am J Sports Med. 2022;50:3487-92.
- [CrossRef] [PubMed] [Google Scholar]
- Anterior cruciate ligament revision plus lateral extra-articular procedure results in superior stability and lower failure rates than does isolated anterior cruciate ligament revision but shows no difference in patient-reported outcomes or return to sports. Arthroscopy. 2023;39:1088-98.
- [CrossRef] [PubMed] [Google Scholar]
- Peroneus longus graft harvest: A technique note. Indian J Orthop. 2023;57:611-6.
- [CrossRef] [PubMed] [Google Scholar]
- Lateral extra-articular tenodesis with iliotibial band using knotless all-suture anchor femoral fixation. Arthrosc Tech. 2023;12:e677-82.
- [CrossRef] [PubMed] [Google Scholar]
- Anterior cruciate ligament rehabilitation and return to sport: How fast is too fast? Arthrosc Sports Med Rehabil. 2022;4:e175-9.
- [CrossRef] [PubMed] [Google Scholar]
- Rehabilitation and return to sport testing after anterior cruciate ligament reconstruction: Where are we in 2022? Arthrosc Sports Med Rehabil. 2022;4:e77-82.
- [CrossRef] [PubMed] [Google Scholar]
- Shape-change phenomenon of the knee in LET surgery: Reduced diameter leaflets maybe the solution. Indian J Orthop. 2024;58:1170-1.
- [CrossRef] [PubMed] [Google Scholar]
- After revision anterior cruciate ligament reconstruction, who returns to sport? A systematic review and meta-analysis. Br J Sports Med. 2015;49:1295-304.
- [CrossRef] [PubMed] [Google Scholar]
- There is a minimal difference in ankle functional outcomes after peroneus longus harvest: Systematic review and meta-analysis. Indian J Orthop. 2023;57:1993-9.
- [CrossRef] [PubMed] [Google Scholar]
- Peroneus longus graft harvest does not affect ankle biomechanics: A narrative review. Indian J Orthop. 2024;58:1206-12.
- [CrossRef] [PubMed] [Google Scholar]
- Does the type of graft affect the outcome of revision anterior cruciate ligament reconstruction?: A meta-analysis of 32 studies. Bone Jt J. 2017;99-B:714-23.
- [CrossRef] [PubMed] [Google Scholar]
- Revision ACL reconstruction using quadriceps, hamstring and patellar tendon autografts leads to similar functional outcomes but hamstring graft has a higher tendency of graft failure. Knee Surg Sports Traumatol Arthrosc. 2023;31:2461-8.
- [CrossRef] [PubMed] [Google Scholar]
- Return to sport following revision anterior cruciate ligament reconstruction in athletes: A systematic review. Arthrosc J Arthrosc Relat Surg. 2019;35:2222-30.
- [CrossRef] [PubMed] [Google Scholar]
- The anterolateral complex of the knee: Results from the International ALC Consensus Group Meeting. Knee Surg Sports Traumatol Arthrosc. 2019;27:166-76.
- [CrossRef] [PubMed] [Google Scholar]
- Anterolateral knee extra-articular stabilizers: A robotic study comparing anterolateral ligament reconstruction and modified Lemaire lateral extra-articular tenodesis. Am J Sports Med. 2018;46:607-16.
- [CrossRef] [PubMed] [Google Scholar]
- Biomechanical comparison of anterolateral procedures combined with anterior cruciate ligament reconstruction. Am J Sports Med. 2017;45:347-54.
- [CrossRef] [PubMed] [Google Scholar]
- The role of lateral extra-articular tenodesis in anterior cruciate ligament reconstruction and treatment of rotatory knee instability: A scoping review. Curr Rev Musculoskelet Med. 2023;16:235-45.
- [CrossRef] [PubMed] [Google Scholar]
- Combined anterolateral complex and anterior cruciate ligament injury: Anatomy, biomechanics, and management-state-of-the-art. J ISAKOS. 2023;8:37-46.
- [CrossRef] [PubMed] [Google Scholar]
- Revision anterior cruciate ligament reconstruction using bone-patellar tendon-bone graft combined with modified lemaire technique versus hamstring graft combined with anterolateral ligament reconstruction: A clinical comparative matched study with a mean follow-up of 5 years from the SANTI study group. Am J Sports Med. 2022;50:395-403.
- [CrossRef] [PubMed] [Google Scholar]







